Osteoporosis treatment: what works and what to ask your doctor
Worried about weak bones or a recent low-impact fracture? Osteoporosis treatment aims to cut fracture risk fast and keep bones strong long term. The right plan mixes proven medicines, daily habits, and simple safety steps. Below I’ll walk you through common medical options, practical lifestyle moves, and quick questions to bring to your next visit.
Medical treatments
First-line drugs for most people are bisphosphonates—alendronate, risedronate, and yearly zoledronic acid. They slow bone loss and lower hip and spine fracture risk. Take oral bisphosphonates on an empty stomach with a full glass of water and stay upright for 30–60 minutes to avoid reflux.
Denosumab (Prolia) is an injection every six months that works well when bisphosphonates aren’t tolerated or when rapid fracture risk reduction is needed. Important: if you stop denosumab, your doctor should switch you to a bisphosphonate to prevent quick bone loss.
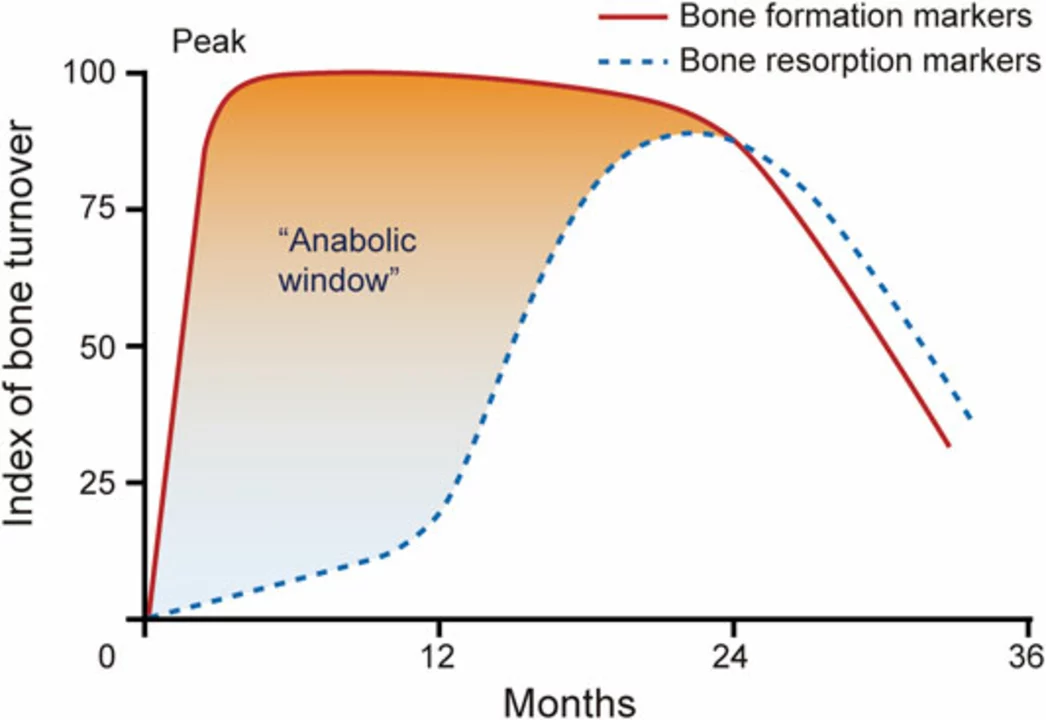
For people with severe osteoporosis or multiple fractures, bone-building drugs like teriparatide or abaloparatide are options. They stimulate new bone formation and are usually limited to 1–2 years. Romosozumab is another newer option that both builds and preserves bone; clinical trials showed it reduced fractures compared with traditional therapy in high-risk postmenopausal women.
Other choices include raloxifene for certain women, and hormone replacement therapy which can help bones but carries other risks to discuss with your doctor. Your personal health, kidney function, fracture history, and preferences decide the best drug for you.
Lifestyle, supplements, and fall prevention
Medicines work best with the right daily habits. Aim for total calcium around 1,000–1,200 mg/day from food first; add supplements only if you can’t meet targets. Vitamin D of 800–1,000 IU/day is commonly recommended for bone health and to reduce falls. Talk to your provider about testing vitamin D levels if you have risk factors.
Do weight-bearing and resistance exercise—walking, stair climbing, light weightlifting—most days. Balance training like tai chi reduces falls. Quit smoking and limit alcohol to lower bone loss.
Falls cause most fractures. Fix loose rugs, add night lights, check footwear, and review meds that cause dizziness. Get your vision checked and consider a home safety review if you’ve fallen before.
Keep track with a DEXA scan to monitor bone density and use tools like FRAX to estimate fracture risk. If you start a drug, stick with it—the biggest gains come from consistent use. Ask your clinician about side effects, how long to stay on treatment, and what to expect if you stop.
If you’ve had a fracture, are over 65, or have a family history of hip fracture, bring that up. Early action prevents more serious breaks later. Treatment choices can be simple but they should match your risks and lifestyle—so ask questions and get a plan you can follow.