Seizure management: Practical steps and treatment options
If you or someone you care for has seizures, you want clear, usable steps—not medical jargon. This guide gives straightforward advice for what to do during a seizure, how to reduce future events, and which treatments doctors commonly use. Use it as a quick reference and share it with family or caregivers.
Quick steps during a seizure
Stay calm. Time the seizure if you can. Move sharp or hard objects away so the person won’t hit them. Cushion their head with a soft object like a folded jacket. Turn the person onto their side to keep the airway clear, unless they have a neck or spine injury.
Do not put anything in the mouth. Don’t try to hold the person down. Speak gently and reassure them as they recover. If the seizure lasts more than 5 minutes, call emergency services—this can be a medical emergency. Also call for help if breathing is difficult after the seizure, if the person is injured, pregnant, or it’s their first seizure.
Long-term management and treatments
Medication is the mainstay of treatment. Anti-seizure drugs (also called antiepileptic drugs) like levetiracetam, valproate, carbamazepine, and lamotrigine are common choices. Which one your doctor chooses depends on seizure type, age, sex, other health issues, and side effects. Take meds exactly as prescribed. Missing doses raises the risk of seizures.
Rescue medications are important for prolonged seizures. Buccal midazolam or rectal diazepam can stop a long seizure while waiting for emergency help. Caregivers should learn how and when to use these. Ask your clinician for a written seizure action plan that lists rescue drug instructions and emergency contacts.
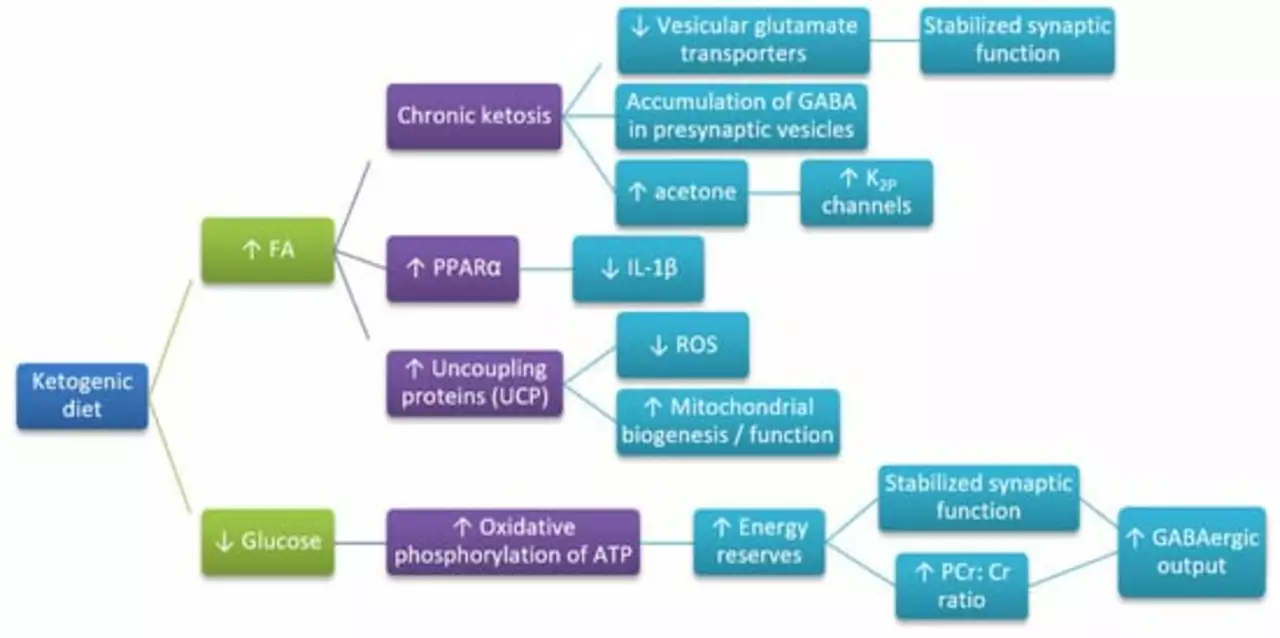
Non-drug options help some people. Vagus nerve stimulation (a small implanted device), responsive neurostimulation, and epilepsy surgery can reduce or stop seizures when medications fail. The ketogenic diet is another option, especially for children with certain epilepsy types. Discuss risks and benefits with a neurologist who specializes in epilepsy.
Lifestyle changes make a real difference. Keep a regular sleep schedule, limit alcohol, manage stress, and follow medication schedules. Identify and avoid triggers if you can—common ones include lack of sleep, flashing lights, missed meds, and high alcohol intake. Use a seizure diary or phone app to track patterns and triggers and bring this to appointments.
Safety at home matters. Install soft furniture edges, avoid swimming alone, and use a shower chair if bathing. Driving rules vary; check local laws and talk with your doctor before getting back behind the wheel.
Finally, stay connected to care. Regular follow-ups, EEGs, and medication reviews help keep seizures under control. If seizures continue despite treatment, ask for a referral to an epilepsy center. With the right plan, many people cut seizures down or stop them entirely—and live full, active lives.