Epilepsy: Practical Guide to Symptoms, First Aid, and Treatment
About 1 in 26 people will develop epilepsy at some point. If you or someone you care for has seizures, knowing the basics makes a big difference. This page gives clear, usable info: how to spot different seizures, simple first-aid steps that work, common treatments, and safety tips you can use right away.
How to recognize seizures and common types
Not all seizures look the same. Two broad groups matter most: generalized seizures and focal (partial) seizures. Generalized seizures often involve loss of consciousness and whole-body jerking. Absence seizures are brief blanking out or staring spells. Focal seizures start in one part of the brain and may cause twitching, strange sensations, sudden emotions, or confusion without losing awareness.
Useful signs: sudden collapse, rhythmic jerking, drooling, frothing, confusion after the event, or brief staring spells. If a spell is new, especially in an adult, get medical help—first seizures need evaluation.
First aid: what to do during and after a seizure
Keep it simple and calm. Follow these steps:
- Protect the person from injury: move sharp objects away and cushion their head. Don’t restrain the jerking.
- Time the seizure. If it goes longer than 5 minutes, call emergency services.
- Roll them gently onto their side as soon as jerking stops so saliva can drain and they can breathe more easily.
- Don’t put anything in their mouth. Don’t try to force their jaw open.
- Stay with them until fully awake and oriented. Reassure them; confusion and tiredness afterward are normal.
Call an ambulance if the seizure lasts over 5 minutes, if breathing doesn’t resume, if another seizure follows quickly, if the person is injured, pregnant, diabetic, or if it’s their first seizure.
Managing epilepsy day-to-day
Most people with epilepsy control seizures with medication. Common drugs include levetiracetam, lamotrigine, carbamazepine, and valproate. Each drug has pros and side effects—work with a neurologist to find the right one. Never stop meds suddenly; that can trigger more seizures.
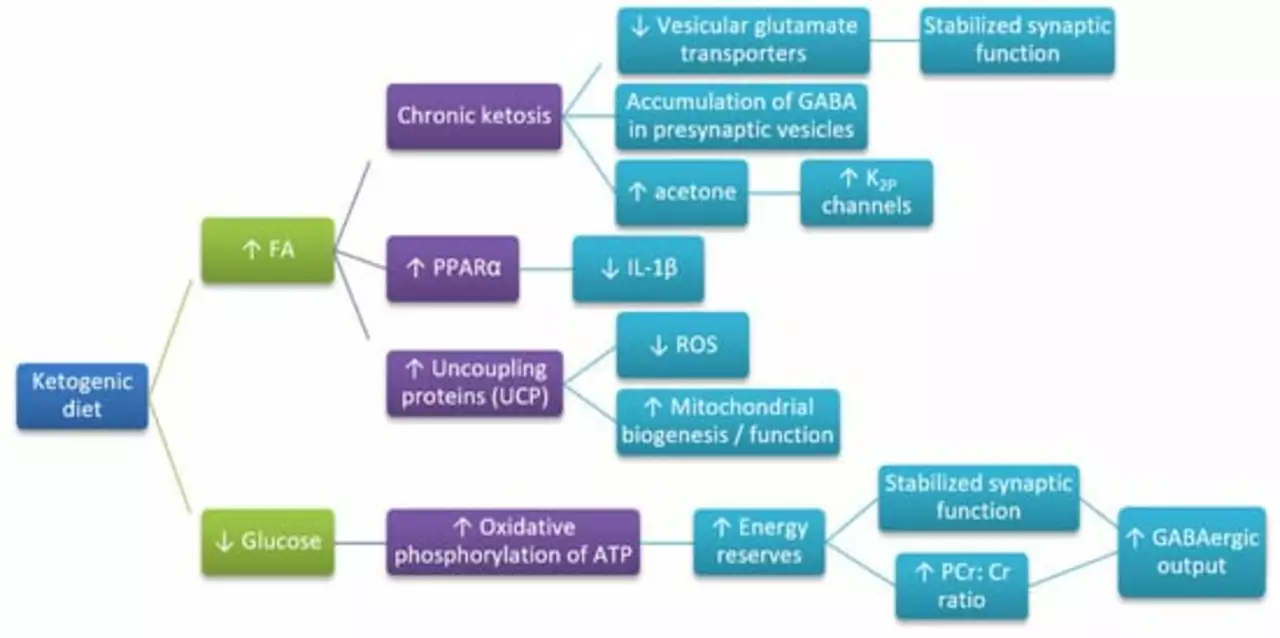
When meds don’t work, other options exist: epilepsy surgery for a clearly localized brain focus, vagus nerve stimulation (VNS), responsive neurostimulation (RNS), or dietary approaches like the ketogenic diet for some children and adults. Your specialist can explain which fits your situation.
Reduce triggers: prioritize sleep, avoid heavy alcohol and recreational drugs, manage stress, and note any patterns (flashing lights, missed meds, illness). Keep a seizure diary—time, activity, possible triggers, and recovery details help your care team adjust treatment.
Safety and planning
Talk to your doctor about driving, workplace safety, and pregnancy planning. Some medications (notably valproate) have higher risks in pregnancy and need careful counseling. Carry a medical ID or note with emergency contact and medication details.
If you want a printable seizure-first-aid checklist or a simple diary template, check resources from your neurologist or epilepsy support groups. Small steps—timers, consistent meds, a safety plan—make life more predictable and safer for people living with epilepsy.